Breakthrough cardiac arrest treatment with the first intelligent fluoroscopy-free balloon catheter
Saving hearts and minds
Neurescue is a medical device startup pioneering an improved treatment of cardiac arrest, the leading cause of death in the world.
About Neurescue
Neurescue is developing cardiovascular devices to help emergency patients. We are passionate about using technology to enable life-saving procedures. Our first product, the NEURESCUE device, is the world's first intelligent fluoroscopy-free aortic balloon catheter with unprecedented safety features, including pressure-controlled inflation and positioning feedback.
Aortic balloon occlusion
1.
The NEURESCUE device is used to inflate a balloon in the descending aorta through a femoral artery introducer sheath. It is the world’s first intelligent balloon catheter for temporary aortic occlusion.
2.
Temporary aortic occlusion is an emergency technique that supercharges blood flow to the heart and brain within one minute from deployment. The NEURESCUE device's simple design is optimized for emergency situations.
3.
This can increase the chance of immediate resuscitation, and bridge the patient to additional life-saving treatment options, such as surgery, PCI, heart-lung machine, and more.
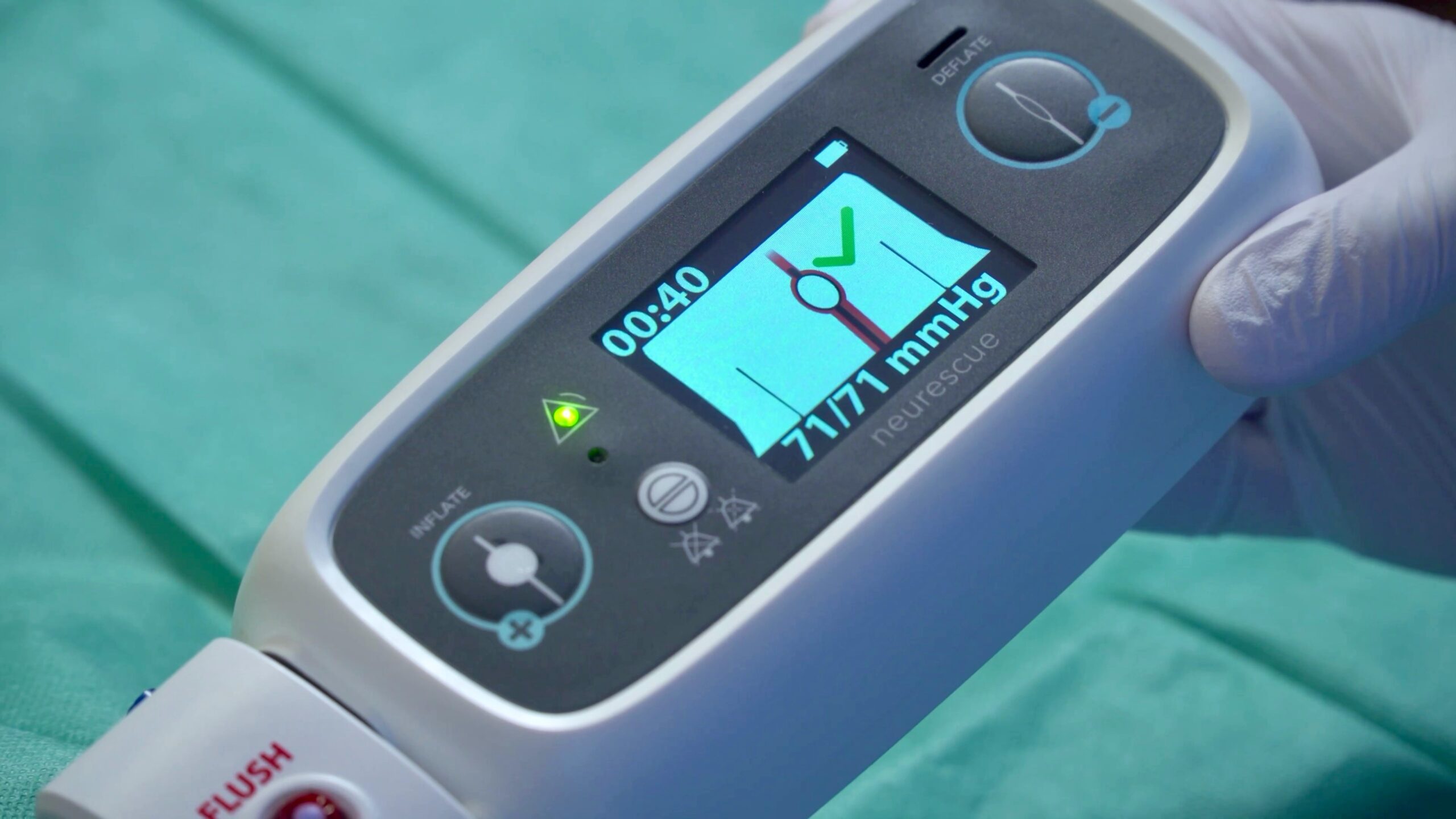
The Neurescue Device is the first computer-aided aortic occlusion catheter, designed to increase blood flow to the brain and heart during life-threatening emergencies. The company has been awarded several innovation awards and large grants by the European Commission and the Danish Innovation Fund.
Only one out of ten cardiac arrest victims survive today
Current standard of care does not reach high enough blood flow to resuscitate most patients. Neither does it buy enough time for more advanced treatment of the patient, such as heart-lung machine. Neurescue seeks to address this unmet need with next-generation medical technology.
20%
Cardiac arrest is a major health problem accounting for an estimated 15-20% of all deaths.
50%
In the United States 40-50% of all lost life years from heart disease is due to cardiac arrest. Cardiac arrest is leading cause of lost life years within heart diseases.
35%
Today's CPR only replaces 35% of blood flow, which is not enough to resuscitate most patients; and does not buy enough time to bridge patients to advanced treatments.
Our solution
The NEURESCUE Device offers a breakthrough intelligent & fluoroscopy-free balloon catheter, allowing for safe aortic occlusion to redirect blood flow to the brain & heart for cardiac arrest patients; intending to 1) allow more patients to achieve immediate resuscitation from cardiac arrest 2) bridging many more patients to definitive treatments intra-arrest - such as ECMO, stents, pacemakers and more.
Within the current standard of treatment, there are no alternatives for the majority of patients who do not respond to CPR and defibrillation. The sensor-guided system helps facilitate a safe procedure for emergency patients. The portable device can be used both inside and outside hospitals.
The NEURESCUE Device is the first computer-aided aortic occlusion catheter, with intelligent safety feedback & pressure-controlled inflation. This allows physicians to insert and inflate a balloon in the aorta, which temporarily redirects blood flow to the brain & the heart of the patient, where it is needed the most. This increases the chance for both immediate resuscitation, while also adding up to one hour to treat the patient definitively with advanced treatments.
Want to know more?
Don't hesitate to get in touch.

This project has received funding from the European Union's Horizon 2020 research and innovation program under grant agreement No 811866
DK OFFICE
Antonigade 11, 2nd floor,
1106, Copenhagen
UK OFFICE
45 Albemarle Street, 3rd floor,
Mayfair, W1S 4JL, London
Saving hearts and minds